香港唯爾醫務中心
全方位的醫療服務中心
![]()
![]()
![]()
查詢或預約Enquiry or Appointment
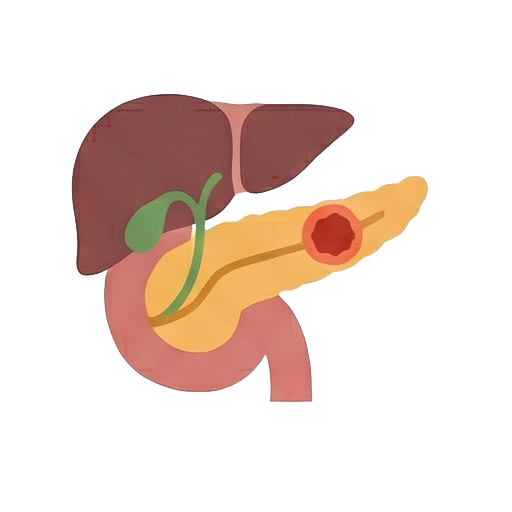
Pancreatic Cancer is widely regarded in the medical community as the “King of Cancers” due to its exceptionally high mortality rate. The pancreas is a long, flat gland situated deep within the abdomen, hidden behind the stomach and in front of the spine. It performs two life-sustaining functions: secreting digestive enzymes to break down food (exocrine function) and producing hormones like insulin to regulate blood sugar (endocrine function).
The danger of pancreatic cancer lies in its stealth. Its deep location means that early, microscopic tumors cannot be felt during routine physical exams or easily seen on standard ultrasounds. Furthermore, the pancreas is surrounded by a dense network of major blood vessels and lymph nodes, allowing cancer cells to spread (metastasize) rapidly to the liver, lungs, or abdominal cavity at a very early stage. Currently, only about 20% of patients are diagnosed early enough for surgical removal, making awareness of risk factors and subtle warning signs absolutely critical for survival.
While the exact cause is not fully understood, medical research has identified several factors that significantly increase the risk:
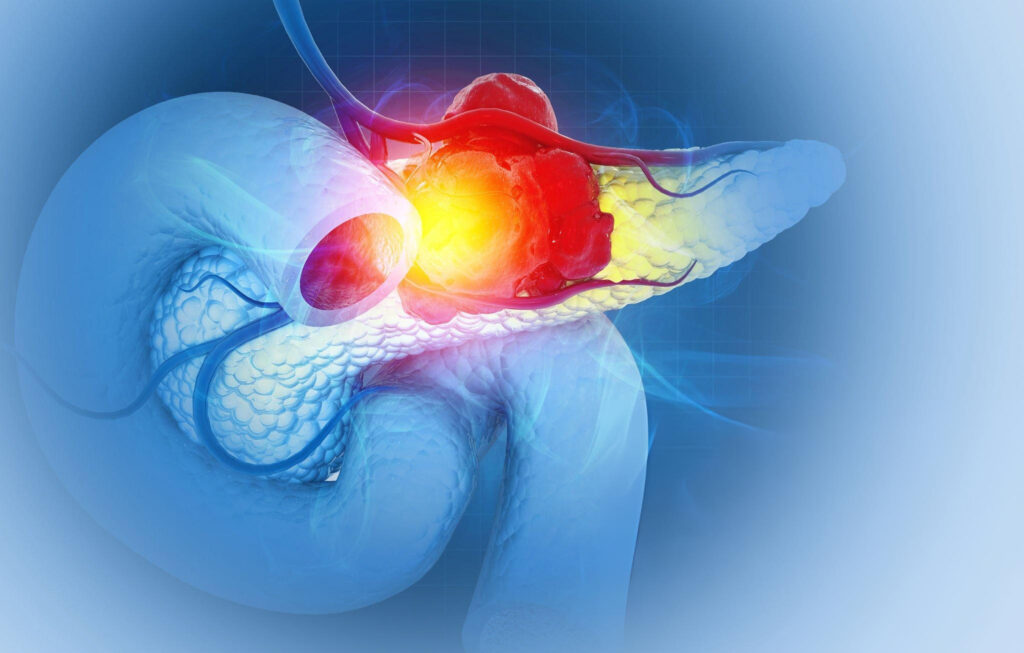
Symptoms vary significantly depending on whether the tumor is located in the “head,” “body,” or “tail” of the pancreas. Be highly alert to the following, especially if they occur together:
Standard abdominal ultrasounds are often obscured by stomach gas, making the pancreas invisible. Specialists must rely on advanced imaging:

Treating pancreatic cancer is extraordinarily complex and requires a coordinated team of hepato-pancreato-biliary (HPB) surgeons and oncologists:
1. Surgery (The Only Curative Option)
Only about 20% of tumors are localized and resectable at diagnosis. The type of surgery depends on the tumor’s location:
– The Whipple Procedure (Pancreaticoduodenectomy): For tumors in the head of the pancreas. This is one of the most complex and demanding operations in all of surgery. It involves removing the head of the pancreas, the duodenum, the gallbladder, part of the bile duct, and sometimes part of the stomach, followed by intricate reconstruction of the digestive tract.
– Distal Pancreatectomy: For tumors in the body or tail, the tail and body of the pancreas are removed, usually along with the spleen.
2. Chemotherapy
Because pancreatic cancer is highly prone to micro-metastasis (invisible early spread), systemic chemotherapy is a cornerstone of treatment.
– Neoadjuvant Chemotherapy: Given before surgery to shrink borderline-resectable tumors, pulling them away from major blood vessels to make surgery possible.
– Adjuvant Chemotherapy: Essential after surgery to eradicate microscopic remaining cells and delay recurrence.
– Palliative Chemotherapy: The standard of care for advanced/metastatic disease, utilizing powerful combinations to control growth, relieve symptoms, and extend survival.
3. Radiotherapy
Often combined with chemotherapy (chemoradiotherapy) to treat locally advanced tumors that cannot be surgically removed but haven’t spread to distant organs. It is also highly effective at shrinking tumors that are causing severe pain by pressing on spinal nerves.
4. Targeted Therapy and Genetic Testing
Precision medicine is making inroads. If genetic profiling reveals specific inherited mutations (like the BRCA mutation), oncologists can prescribe targeted oral drugs (PARP inhibitors) as maintenance therapy, offering a new lifeline for certain advanced patients.

![]()
![]()
![]()

