香港唯爾醫務中心
全方位的醫療服務中心
![]()
![]()
![]()
查詢或預約Enquiry or Appointment
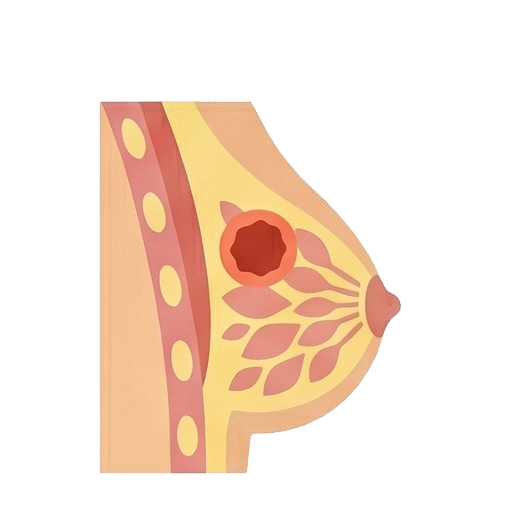
Breast Cancer is the most common cancer among women in Hong Kong and the third leading cause of cancer-related deaths for women in the region. It occurs when cells in the breast tissue (such as the ducts or lobules) undergo genetic mutations, lose control over their normal growth, and multiply abnormally to form a malignant tumor. Although the vast majority of breast cancer patients are women, men also have breast tissue and can, in rare cases, develop breast cancer.
According to the latest data from the Hong Kong Cancer Registry, the number of new breast cancer cases has been continuously rising, with a trend of affecting younger women. However, thanks to advancements in medical imaging and the introduction of innovative anti-cancer drugs (such as targeted and immunotherapies), the 5-year survival rate for early-stage breast cancer exceeds 90% when detected and treated promptly.
The exact single cause of breast cancer remains unknown, but medical research has identified several interacting factors that significantly increase the risk of developing the disease:
Early-stage breast cancer is often painless, and lumps may be too small to notice. As the tumor grows, patients may observe the following symptoms:

Doctors generally utilize a “Triple Assessment” approach to ensure maximum diagnostic accuracy:
Step 1: Clinical Examination and Medical History
A specialist will review the patient’s detailed medical history and perform a physical examination of the breasts and underarm lymph nodes to check for abnormalities.
Step 2: Medical Imaging
Step 3: Biopsy
If imaging reveals suspicious lesions, a biopsy is performed, most commonly a Core Needle Biopsy. This not only confirms whether the tissue is malignant but also analyzes the tumor’s biological characteristics (such as Estrogen Receptor ER, Progesterone Receptor PR, and HER2 status), providing crucial data for personalizing the treatment plan.
Breast cancer is not a single disease. Pathologists categorize it into major molecular subtypes based on gene expression, which dictates the most effective systemic treatments:
Staging is based on Tumor size (T), Node involvement (N), and distant Metastasis (M):
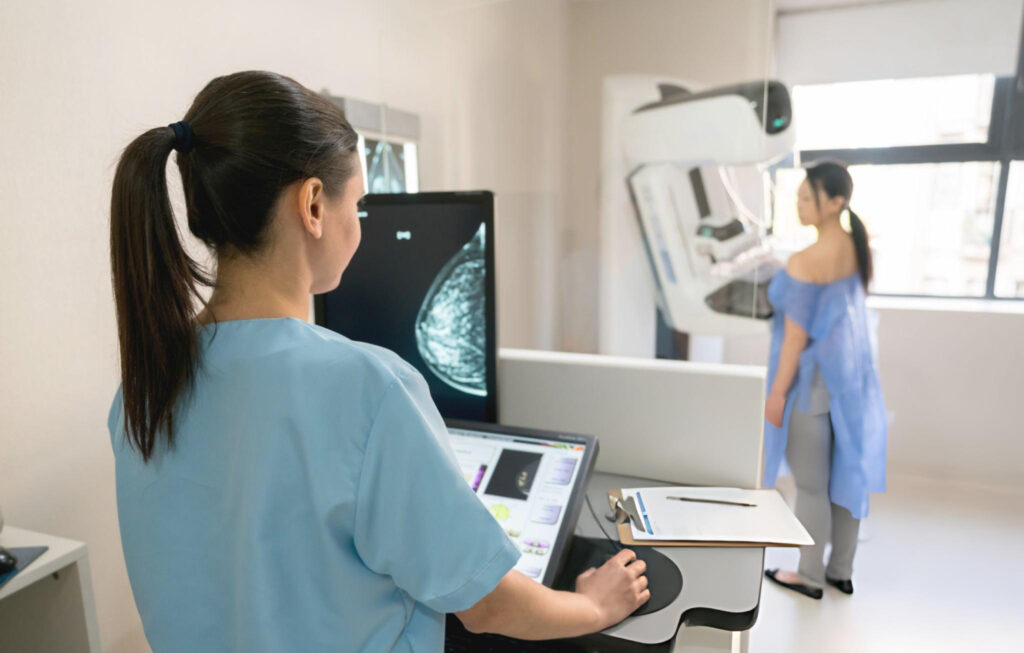
Treating breast cancer involves a highly personalized, multidisciplinary approach, often combining surgery, medical oncology, and radiation oncology:
1. Surgery
Surgery is the primary curative step for early-stage breast cancer. Options include:
2. Radiotherapy
Utilizes high-energy X-rays to destroy cancer cell DNA. It is standard after a lumpectomy to eliminate any microscopic residual disease, or after a mastectomy for high-risk patients to treat the chest wall and regional lymph nodes, significantly lowering local recurrence rates.
3. Chemotherapy
Systemic use of anti-cancer drugs administered intravenously or orally to kill rapidly dividing cancer cells.
– Adjuvant Chemotherapy: Given after surgery to eradicate microscopic metastasis and reduce relapse risk.
– Neoadjuvant Chemotherapy: Given before surgery for large or aggressive tumors to shrink them, especially for HER2-positive and Triple-Negative Breast Cancer (TNBC). potentially allowing a patient who initially needed a mastectomy to become eligible for breast-conserving surgery.
4. Hormonal (Endocrine) Therapy
Used for hormone receptor-positive (ER+/PR+) cancers. Drugs are prescribed to block the body’s estrogen production or receptors (e.g., Tamoxifen for pre-menopausal women, or Aromatase Inhibitors for post-menopausal women). Standard treatment duration spans 5 to 10 years.
For young (premenopausal) female breast cancer patients, the use of “ovarian suppression injections” (GnRH agonists) suppresses estrogen production at its source. By depriving cancer cells of the estrogen they rely on to survive, this approach can significantly reduce the risk of cancer recurrence and metastasis.
5. Targeted Therapy and Immunotherapy
– Targeted Therapy: Specific drugs designed to hone in on molecular targets (like HER2), blocking the signaling pathways that drive cancer growth with less damage to healthy cells.
– Immunotherapy: Drugs that strip away cancer cells’ ability to hide from the immune system, reactivating the patient’s T-cells to track down and destroy the cancer. Currently used mostly for certain TNBC cases and advanced metastatic stages.
6. Antibody-Drug Conjugates (ADC)
Antibody-Drug Conjugates (ADCs) represent one of the most significant medical breakthroughs in the field of breast cancer treatment in recent years. They ingeniously combine the precision of “targeted therapy” with the potent killing power of “chemotherapy.”
–Mechanism of Action: ADC drugs are composed of a “monoclonal antibody” linked to a “potent chemotherapy drug.” The antibody acts as a navigation system, precisely locating and binding to specific receptors (such as HER2) on the surface of cancer cells. Once the ADC enters the cancer cell, it releases a high concentration of the chemotherapy drug, destroying the cancer cell from the inside out. This approach minimizes damage to surrounding healthy cells, usually resulting in milder side effects compared to traditional chemotherapy.
–New Breakthroughs in HER2 Treatment: In the past, anti-HER2 targeted therapies were only effective for “HER2-positive” patients. However, the latest ADC drugs have broken this boundary. For patients previously classified as HER2-negative but who actually express low levels of the HER2 protein—now clinically recognized as “HER2-low”—ADC drugs demonstrate remarkable efficacy, bringing entirely new treatment hopes to a vast number of patients with advanced breast cancer.
–Broad Clinical Applications: Not only are ADCs highly effective in treating advanced or metastatic breast cancer, but recent clinical studies also show immense promise in Neoadjuvant Therapy (treatment given before surgery). Administering ADC drugs pre-operatively can significantly shrink the tumor volume, thereby increasing the success rate of breast-conserving surgery and improving long-term prognostic outcomes.
Regular medical follow-ups, including clinical exams and mammograms, are vital post-treatment to monitor for recurrence. For daily life, we recommend:

![]()
![]()
![]()

