香港唯爾醫務中心
全方位的醫療服務中心
![]()
![]()
![]()
查詢或預約Enquiry or Appointment
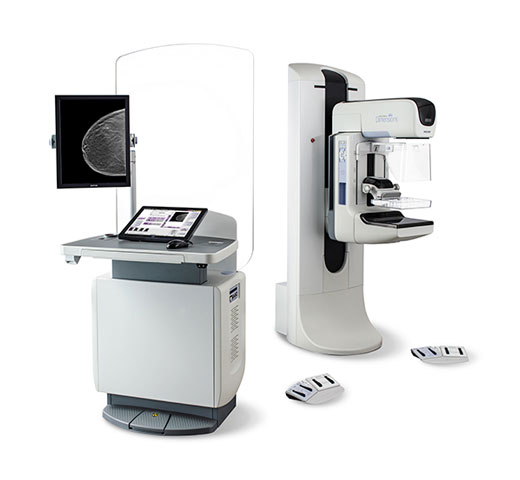
Mammography is the only screening tool medically proven and globally recognized to effectively reduce breast cancer mortality. Whether utilizing traditional 2D or advanced 3D technology, the core strength of mammography lies in its ability to detect tiny, unpalpable tumors and “microcalcifications”—often the only early sign of breast cancer. Early detection and treatment can lead to a survival rate of over 90%.
| Features | Conventional 2D Mammography | 3D Mammography (Tomosynthesis) |
|---|---|---|
| Image Visualization | Single flat plane (Top-to-bottom and side views) | Multiple angles, reconstructed into 1mm thin 3D slices |
| Tissue Overlap Issues | Significant. May hide tumors or create false lesions | Minimal. Layer-by-layer view eliminates overlapping structures |
| Early Cancer Detection Rate | Standard | Significantly higher (Detects up to 40% more invasive cancers) |
| False Positive / Call-back Rate | Higher, often requiring additional imaging | Reduced by 15% – 40%, minimizing patient anxiety |
| Best for “Dense Breasts” | Less effective, diagnosis can be limited | Excellent. The gold standard for Asian women and dense tissue |
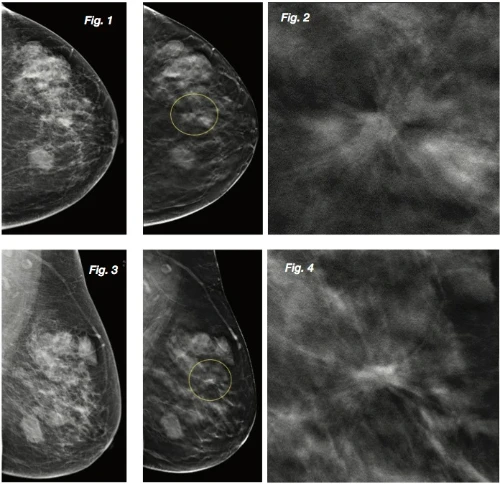
We strongly recommend that women aged 40 and above undergo a routine screening mammogram every 1 to 2 years. If you have any of the following “high-risk factors,” consult your doctor about starting screenings earlier, typically at age 35:
Pain tolerance varies, but most women experience temporary discomfort or pressure. Firm compression is essential for several reasons: it flattens the breast to prevent tissue overlap (uncovering hidden tumors), reduces tissue thickness (significantly lowering the radiation dose required), and holds the breast completely still to prevent blurry images. Our advanced 3D systems use ergonomically curved paddles that distribute pressure evenly, making the procedure much more comfortable than older machines.
Breasts are composed of fat and glandular tissue. If you have more glandular tissue than fat, you have “dense breasts,” which is very common among Asian women. On a 2D X-ray, both dense tissue and tumors appear “white.” Looking for a tumor in a dense breast is often compared to looking for a snowball in a snowstorm. 3D tomosynthesis solves this by slicing through the tissue layer by layer, preventing the white dense tissue from masking underlying tumors.
Absolutely, and it is just as important! Please inform our staff about your implants (silicone or saline) when booking. Our specially trained radiographers will use a technique called “Implant Displaced Views.” They will gently push the implant back against the chest wall and pull the natural breast tissue forward to compress and image it. This ensures the implant remains safe while the breast tissue is thoroughly examined.
They cannot replace each other; they are complementary. Ultrasound is excellent at distinguishing solid lumps from fluid-filled cysts without radiation. However, ultrasound is very poor at detecting “microcalcifications,” which are often the very first and only sign of early-stage breast cancer. Mammography is the gold standard for finding these calcifications. For women over 40, using both methods together provides the most comprehensive and accurate screening.
It is extremely safe. Modern digital mammography utilizes a very low dose of radiation. The dose for a standard two-view bilateral mammogram is about 0.4 millisieverts (mSv), which is roughly equivalent to the natural background radiation you absorb from your environment over 7 weeks, or the exposure during a long-haul flight. The risk of harm is almost negligible, while the life-saving benefits of early breast cancer detection are immense.
If you are pregnant or suspect you might be, you should NOT have a mammogram due to potential radiation risks to the fetus; consult your doctor about a breast ultrasound instead. If you are breastfeeding, mammograms are safe, but your breasts will be filled with milk, making the tissue extremely dense and the images very difficult to read accurately. It is generally recommended to wait at least 3 months after you have completely stopped nursing to have a screening mammogram.

![]()
![]()
![]()

